For a widow who has outlived many of her friends, loneliness can make managing a chronic condition even worse. This is the case for Cynthia, a 75-year-old patient with a new diagnosis of congestive heart failure and stage 3 renal disease. Cynthia recently lost her husband and several of her closest friends. She has found herself bouncing back and forth from skilled nursing facility to home and has found it increasingly difficult to stay on top of her medication schedule by herself.
Long before the COVID-19 pandemic, older adults experienced the ill effects of social distancing. The American Psychological Association characterizes this social isolation and loneliness among seniors as a deadly epidemic. Not only feeling lonely, isolated seniors were also suffering from physical and mental health problems from depression to Alzheimer’s disease.
To better understand the epidemic, the University of Michigan surveyed around 2,000 Americans between the ages of 50 and 80. This 2019 National Poll on Healthy Aging, sponsored by AARP, revealed that one in three seniors feel lonely at least sometimes. One in four connect with others either once per week or not at all, making them socially isolated. In February 2020, a report by the National Academies of Sciences, Engineering and Medicine, also sponsored by AARP, found that 43% of adults over 60 feel lonely.
What causes loneliness in seniors?
Societal changes are partly to blame for the loneliness epidemic, according to research published in BMC Public Health. Seniors are more likely to live separate from their children. They’re also less likely to be integrated into their communities. Plus, medical advancements have led to longer lifespans, allowing more time for negative outcomes to arise.
Loneliness rarely results from a single cause. America’s Health Rankings suggests a handful of risk factors:
- Living alone is a risk factor, as are social determinants like age, gender, race, ethnicity, sexuality, and income. Women report feeling lonelier than men, for example.
- Certain health conditions put seniors at risk. Hearing loss, in particular, seems to have a negative impact. In the above-mentioned University of Michigan poll, lonely and socially isolated seniors were nearly twice as likely to report hearing issues than their peers.
- Life events also have an impact. Losing a significant other, whether a spouse or close friend, leads to feelings of loneliness. Retiring from the workforce has a similar impact, as does losing one’s driver’s license.
When epidemic and pandemic collide
The COVID-19 pandemic is exacerbating the existing loneliness epidemic in seniors. Seemingly overnight, avenues for social contact have disappeared, leaving most seniors, if not all, feeling disconnected.
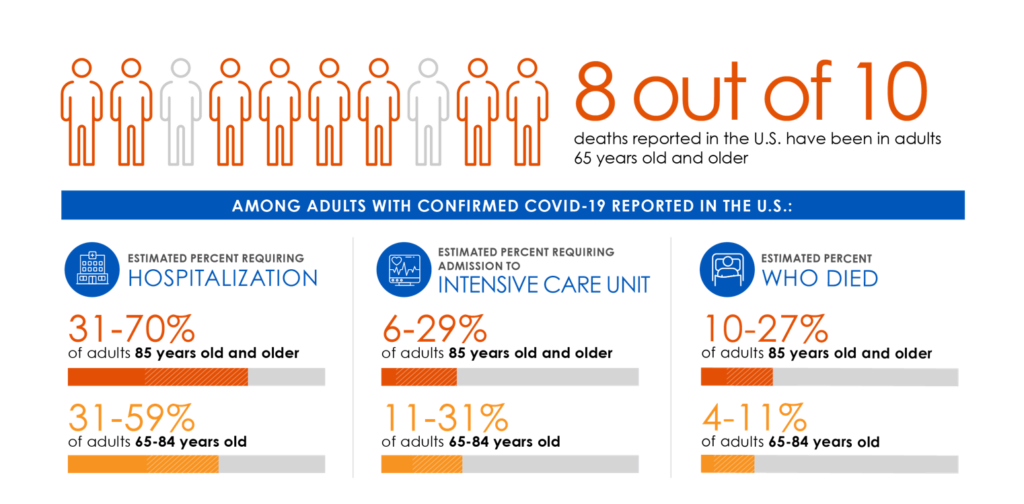
The Centers for Disease Control and Prevention (CDC) say seniors are at elevated risk for catching the SARS-COV-2 virus, and report that adults over 65 account for eight in 10 deaths from the virus. Because seniors are at higher risk than their younger peers, the CDC recommends they stay home and keep their distance from others.
As a result, governments have temporarily closed community centers, public libraries and places of worship, banned visitors from nursing homes and restricted restaurants to takeout and delivery services. While their intentions are in the right place, they’ve inadvertently placed a generation of seniors at higher risk for the negative health outcomes associated with loneliness.
Being socially isolated and feeling lonely puts seniors at risk for early death. In the above-mentioned University of Michigan poll, lonely seniors were twice as likely to report fair or poor physical health than those who felt connected to others. Strikingly, 17% of socially isolated seniors reported fair or poor mental health compared to just 2% of those with regular social contact.
Prolonged isolation is comparable to smoking 15 cigarettes per day, according to Connect2Affect, a campaign spearheaded by the AARP. Plus, loneliness has a larger impact on seniors than being obese or leading a sedentary lifestyle, according to research published in BMC Public Health.
Negative health outcomes include chronic inflammation, a weakened immune system, hypertension, and heart disease. Loneliness in seniors is also correlated with depression, anxiety and cognitive decline — according to the National Institute on Aging. In fact, the National Academies of Sciences report suggests lonely seniors are 1.5 times as likely to get Alzheimer’s disease.
Should healthcare organizations intervene?
Alongside the report cited above, the National Academies of Sciences released a position statement concerning loneliness in seniors; the statement argued that health systems are an under-utilized resource when it comes to addressing socially isolated seniors.
The group points out that, for socially isolated seniors, “a medical appointment or home health visit may be one of the few social interactions they have.” As a result, healthcare professionals are uniquely positioned to tackle the epidemic of loneliness in seniors.
The multitude of risk factors is problematic for designing interventions. Most experts agree that treatments must be tailored to each individual, or at least to groups of individuals who share the same risk factors and degree of loneliness. Comprehensive assessments that allow practitioners to carve out groups of seniors based on their risk factors are thus key.
It may not seem like a lot, but a simple interaction may help lift a senior patient’s spirits significantly. For Cynthia, one of those simple interactions was a phone call from Crystal, a clinician from Cynthia’s rehabilitation facility. Cynthia was calling to see how Crystal was doing back at home. Cynthia admitted that being home was more difficult than she thought it would be – and that she couldn’t remember which medications to take and at what time. She was even considering going to the emergency room if she didn’t feel better by the end of the week.
Not only was Crystal able to assist Cynthia in getting back on track based on her original discharge plan, but she also followed up with Cynthia’s primary care physician. That simple interaction provided Cynthia with the help that she needed, but it ultimately helped stop an unnecessary readmission as well.
It’s these types of interactions that include clinical and non-clinical questions that will allow patients like Cynthia to overcome their feelings of loneliness in the world. In today’s COVID-19 climate, it may be even more important to not only help patients through a successful care transition back to their home but to lend an ear and a familiar voice to those who need it most.
Listen to naviHealth infectious disease and healthcare experts Ken Botsford MD and Shelli Lara, as they rethink care amidst the current COVID-19 climate and offer high-touch non-clinical, home-based approaches and best practices for healthcare providers.



